Ear Infections
Any time someone has prolonged pain in their ear, they may think they have an ear infection. What most people don’t realize is that, just like there are multiple parts of the ear, there are multiple types of ear infections. Fortunately, as ear, nose, and throat specialists, we can help diagnose your ear problem and deliver an effective treatment.
External Ear Infections
The outer portion of the ear that you can actually see on the sides of your head is referred to as the auricle or pinna. This part of the ear can become infected due to bug bites, external trauma from due to sports or fights, or piercings. Since this area is visible to the naked eye, it is typically easy to identify the issue.
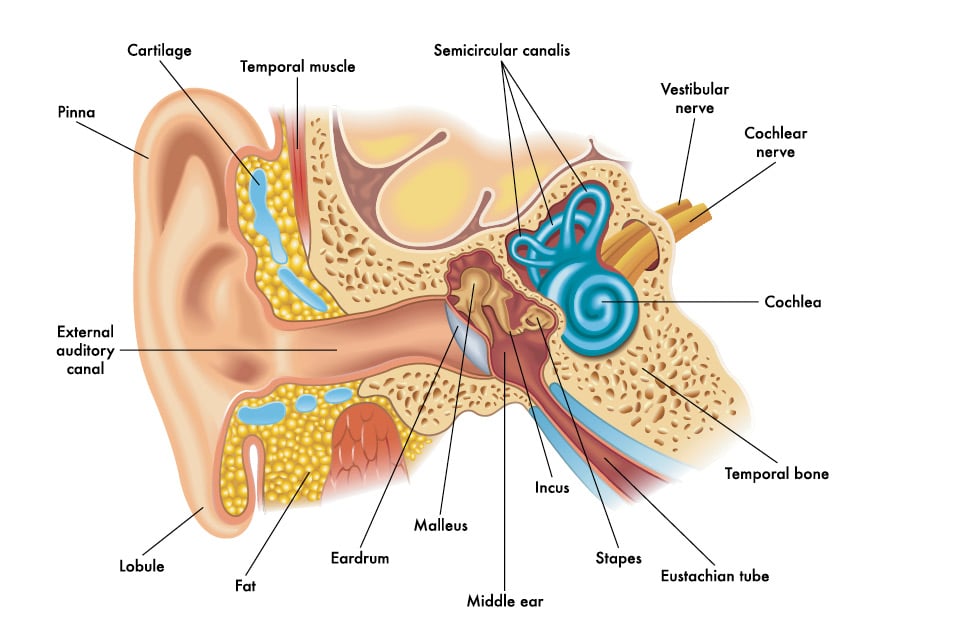
The external auditory canal is also considered part of hte external ear, even though it extends inward to the eardrum. Swimmer’s ear (otitis external) and fungal infections can occur in this area of the ear.
Swimmer’s Ear
Sometimes excessive earwax can trap moisture, creating a perfect environment for bacteria to grow and cause otitis externa. In other instances, trauma to the ear canal can occur from Q-tips, pencils, fingers, paperclips, or bobby pins. Even slight pressure can result in a scratch on the very thin skin of the ear canal, leading to an infection. Otitis external is often called swimmer’s ear because it’s related to swimming and then feeling like water was still in your ear later in the day.
When something like this happens, you may experience fullness and/or slight pressure in the ear for a day or so, and then the pain begins. The ear canal can become swollen, a foul-smelling drainage may occur, the quality of hearing can decline, and pain may continue to progress. Tugging on the earlobe or pressing on the area just in front of the ear canal will often increase the pain.
Most often, the infection can be cured with antibiotic drops that contain a steroid. If the ear canal swelling is excessive, this approach alone may not work. In those cases, referral to an otolaryngologist is very important. The most important next step is to clean the ear of all impacted wax and infected debris. Sometimes an otowick is required to enable the drops to reach the infected area. An otowick is a condensed piece of cotton that is placed in the ear canal to allow the drops to penetrate further down. Another point to keep in mind is whether or not the infection extends outside of the ear canal. If there is swelling in front of the ear, or the outer ear itself becomes red and swollen, then oral antibiotics will typically need to be used in addition to the eardrops.
Fungal Infections
Fungal infections may be referred to as fungal otitis externa, otomycosis, or mycotic otitis externa. A patient with this type of external ear infection may complain of excessive itching, some hearing loss, and ear drainage. Ear canal drainage that results from a fungus may have a thick, white, spongy appearance that can also feature black, yellow, or green specks. Under a microscope, it can look very similar to mold growing on bread. Fungus enjoys warm, dark, moist environments with organic debris present, so ears with flaky skin such as eczema are often infected with fungus, especially after the use of a topical antibiotic drop.
Treatment for these ear infections typically requires removal of the debris in the ear canal and application of antifungal medicine, in either powder or liquid form. Unfortunately, a fungal ear infection can often take longer to resolve, and the ear may need to be cleaned out more than once. In addition, treatment of any underlying eczema or skin condition is necessary to avoid recurrence.

Middle Ear Infection (Otitis Media)
 The technical term for a middle ear infection is otitis media, and this is the type that many patients incorrectly call an inner ear infection. The middle ear is an air-filled space behind the eardrum, and the small bones of the ear are located in this area. This region of the ear does not come in contact with the outside air, so getting water in the ear will not typically result in a middle ear infection. Of course, there are always a few exceptions to this rule. If there is a hole in the eardrum or ear tubes have been placed in the eardrum, then water has a way to get into the middle ear area.
The technical term for a middle ear infection is otitis media, and this is the type that many patients incorrectly call an inner ear infection. The middle ear is an air-filled space behind the eardrum, and the small bones of the ear are located in this area. This region of the ear does not come in contact with the outside air, so getting water in the ear will not typically result in a middle ear infection. Of course, there are always a few exceptions to this rule. If there is a hole in the eardrum or ear tubes have been placed in the eardrum, then water has a way to get into the middle ear area.
The middle ear is connected to the back of the throat and nose area by a structure called the Eustachian tube. If you have ever heard a doctor or nurse say something like, “your tube is blocked or not working,” this is what he or she was referring to. The purpose of the Eustachian tube is to equalize the pressure in the middle ear. This most commonly happens briefly during swallowing and can be heard as faint clicking sounds even when healthy people swallow. An example of the Eustachian tube working properly is what happens when you go up in the mountains, an airplane, or an elevator. Your hearing may start to become muffled in these scenarios, but it will typically go back to normal once you swallow or “pop your ears.” That is your Eustachian tube at work! When it does not work because it is swollen due to a virus or allergy, for example, then the middle ear pressure becomes lower than that of the outside world, which causes the eardrum to be sucked in and causes mucus or “fluid” to fill the middle ear. If there is an infection, this is called acute suppurative otitis media. If there is no infection, it is called acute serous otitis media.
Middle ear infections are frequently diagnosed in young children, and one of the main causes is fluid accumulation because the Eustachian tube is not working properly. This fluid may become infected with bacteria. Most of the time, middle ear fluid will resolve on its own without treatment. However, if it becomes infected, an oral antibiotic is usually required. Additionally, if the infections or episodes of fluid buildup become very frequent or the fluid does not go away for several months, tubes can be placed in the eardrum to resolve the ventilation problem and restore normal air pressure to the middle ears. Known as myringotomy tubes, pressure equalization tubes or pneumatic equalization tubes (PE tubes in all cases), these tubes connect the middle ear space with the external canal to help ensure the pressure behind the eardrum equals that of the outside air.
Inner Ear Infections
An inner ear infection is the scariest type of ear infection, and the term is also the most wrongly overused in the healthcare system. The inner ear is the part of the ear that is closest to the brain, and it contains fluid that is in communication with the fluid surrounding the brain. Inflammation or infection in these areas can result in vertigo (a spinning sensation associated with nausea and vomiting), loss of balance, and even permanent hearing loss. It is also worth noting that infections of the inner ear are usually from a virus and much less commonly from bacteria. There are actually two main types of inner ear infections, labyrinthitis and vestibular neuritis.
Labyrinthitis
Labyrinthitis is an infection of the fluid in the inner ear that can affect a patient’s balance and ability to hear. These can be devastating infections, often permanently damaging the nerves in the inner ear that control hearing and balance functions.
Vestibular Neuritis
In contrast, vestibular neuritis is inflammation of the nerve branch that is associated only with balance. Therefore, the symptoms of vestibular neuritis are dizziness or vertigo, but there would be no change in hearing. In addition, neuritis is far more commonly a viral infection and thus often self-limited and temporary in its symptoms.
Vestibular neuritis symptoms typically occur suddenly and last 24-48 hours before they begin to slowly improve. However, some symptoms can last up to several weeks and include chronic dizziness, disorientation, and difficulty concentrating. Medications to control nausea and help decrease the sensation of vertigo are often prescribed. Steroid medication can also be used to decrease inflammation, and antibiotics can help treat a bacterial infection. If nausea is severe enough to cause dehydration, hospitalization may be required.
Bacteria From The Middle Ear
Sometimes a severe middle ear infection can result in some toxins passing into the inner ear fluid, and this can result in mild problems with balance. If bacteria successfully make their way into the inner ear fluid, permanent hearing loss and permanent damage to the inner ear can occur. Since this fluid is connected to the fluid around the brain, it can lead to bacterial meningitis if left untreated, which can be fatal.
Ramsay Hunt syndrome
Lastly, there is an unusual viral infection that travels along the nerves themselves and thereby affects both the inner and external ears. This is a form of “shingles” or secondary varicella zoster infection called Ramsay Hunt syndrome. It is quickly identified by the combination of vertigo, hearing loss, and a finding of blisters on the external ear (often located in the concha immediately adjacent to the entrance of the ear canal). Any case of suspected Ramsay Hunt syndrome should be referred to an otolaryngologist immediately for emergency treatment to avoid permanent facial paralysis, hearing loss, and balance problems.





