Thyroid Nodules
Thyroid nodules, sometimes known as goiters, are a common and usually harmless phenomenon that involves a growth of cells within the thyroid gland. However, in some cases, a thyroid nodule may be something more serious, such as cancer or cells that elevate thyroid hormone levels, and thus pose a health risk. In these cases, a thyroid nodule may require the attention of a surgical specialist, usually an otolaryngologist (ENT doctor) experienced in treating disorders of the thyroid and parathyroid glands.
Thyroid nodules need to be of a certain size to be felt in the neck, usually larger than a centimeter and often around 2 centimeters to be easily felt. This is because the gland is deep in the neck and covered by other tissues that obscure these nodules. As a result, thyroid nodules are often missed on routine neck exams.

Single Thyroid Nodule or Dominant Thyroid Nodule?
If there are multiple nodules it is known as a multinodular goiter. If a single nodule or dominant (largest) nodule in a multinodular goiter is identified, more testing is needed to make sure it is not cancerous. Patients would typically be referred to an otolaryngologist with experience in head and neck surgery to evaluate the nodule and to determine if a biopsy and possibly surgical removal is appropriate. An endocrinologist is usually involved in this process to monitor or adjust a patient’s thyroid function and hormone levels, as well as to obtain biopsies of any suspicious nodule.
Discovering The Thyroid Nodule
This process often begins with the discovery of a nodule during a physical exam or as an incidental (unexpected) finding on imaging of the head and neck such as a neck CT scan or MRI. Thyroid nodules are rarely large enough to cause pain, discomfort, or visible swelling in the neck. Once a nodule is found, thyroid function blood tests and imaging are usually recommended to better understand any potential risks to your health. The results of the thyroid function blood tests will help the physician decide which type of imaging study is needed. A nuclear scan of the thyroid is usually recommended for patients with elevated thyroid function levels (hyperthyroidism). An ultrasound examination is usually recommended for patients with normal or low thyroid function levels (hypothyroidism).
Nuclear Scans
With a nuclear scan, the patient is given a pill containing a special radioactive dye that is taken up by the thyroid gland. The levels of radiation are very low and therefore safe for the patient. A scan is then performed to study the gland to look for unusual patterns of the dye. If the dye is taken up extensively by the nodule, it is almost always benign. Decreased uptake of dye into the nodule may be a sign of thyroid cancer. In cases like this, an ultrasound and eventual biopsy are usually performed. Because most nodules are found in patients with normal or low thyroid hormone, and because the technology has improved so much with ultrasound imaging, nuclear scans are not performed as often as they once were.
Thyroid Nodule Ultrasound
Thyroid nodules are notoriously difficult to feel and accurately assess on a physical examination alone. In many cases, an enlarged thyroid is caused not just by a single nodule, but rather by several smaller nodules spread throughout the thyroid gland. An ultrasound exam can reveal the size, number, location, and appearance of thyroid nodules in detail, using ultra-high-frequency sound waves that are harmless to the human body. The exam is completely painless and typically only takes about 30 minutes. Sedation is not required because there is no discomfort. After the exam, a radiologist and your surgeon will review the images.
The ultrasound can examine and identify certain features of the nodule that indicate whether a nodule is likely to be harmless, or possibly be a concern for cancer. These features include the shape or texture of a nodule, the presence of calcium deposits, levels of blood flow within the nodule, the presence of a fluid cyst within the nodule, or growth and spread of the nodule beyond the edge of the thyroid gland. The ultrasound exam can also evaluate the lymph nodes surrounding the gland to see if they are normal in appearance. A biopsy will usually be recommended for nodules that are growing quickly, nodules larger than 2 cm in size, or nodules that are smaller, but appear abnormal on the ultrasound.
In some cases, multiple nodules may be seen on ultrasound. These are collectively referred to as a “multinodular goiter.” If one of these nodules is significantly larger than the others, it is known as a “dominant nodule” and is considered to be at higher risk for malignancy. Dominant nodules are often biopsied for this reason.
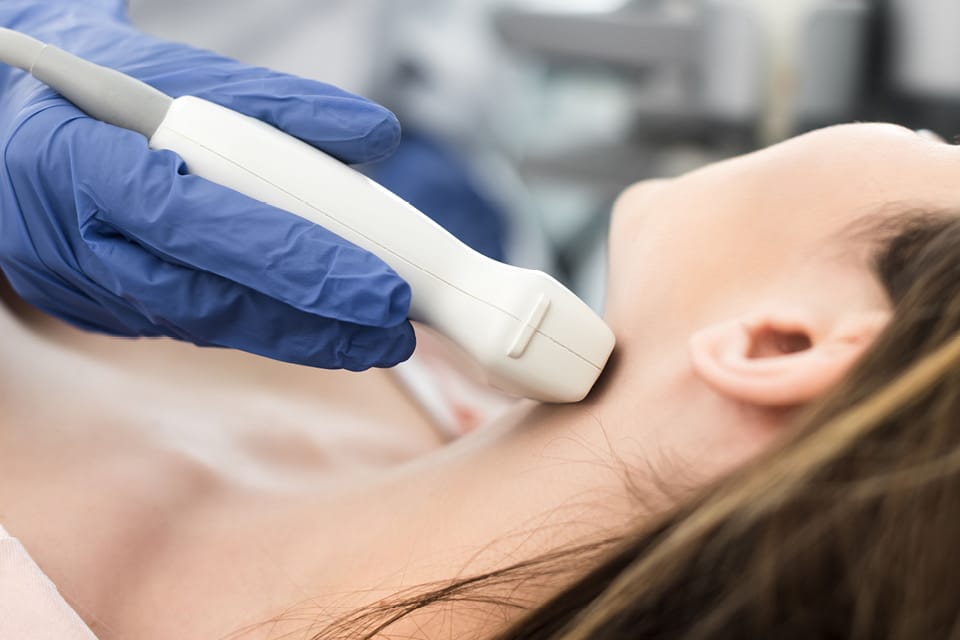
Fine-Needle Aspiration Biopsy
If an abnormal nodule is evident after imaging, a fine-needle aspiration (FNA) biopsy is usually ordered due to the possibility of thyroid cancer. This procedure involves the passage of a small hollow needle into the nodule. The needle is attached to a syringe, which is used to draw small clumps of cells into the needle from the nodule. Because only a small portion of a nodule may contain cancer, this process is often repeated three or more times to ensure that tissue is sampled from all areas of the nodule. The FNA biopsy is typically performed in an outpatient office setting by a surgeon, radiologist, or endocrinologist with specific training and experience. The physician will typically use ultrasound imaging to guide the biopsy needle and ensure that all areas of the nodule are sampled. The test can be a bit uncomfortable, but anesthesia/sedation is not required and there is minimal pain. The process typically takes 30-60 minutes and results are usually available within a week.
Thyroid Nodule Biopsy Results
Thyroid FNA biopsy results usually fall into one of the following six major categories (in order of level of concern) based on the appearance and quality of the cells obtained:
- Benign
- Non-diagnostic
- Atypical cells or follicular lesion of undetermined significance
- Follicular neoplasm/suspicious for follicular neoplasm
- Suspicious for malignancy
- Malignant
The biopsy results will help inform your surgeon of your risk for thyroid cancer. For the lower-risk categories, a simple follow-up thyroid scan may be all that is necessary. In other cases, a repeat biopsy may be recommended. For higher-risk categories, your surgeon will usually recommend thyroid surgery.
The ear, nose, and throat specialists at CornerStone Ear, Nose & Throat have years of experience performing thyroid surgery and helping patients with thyroid nodules. To learn more or to make an appointment, call 704-752-7575.